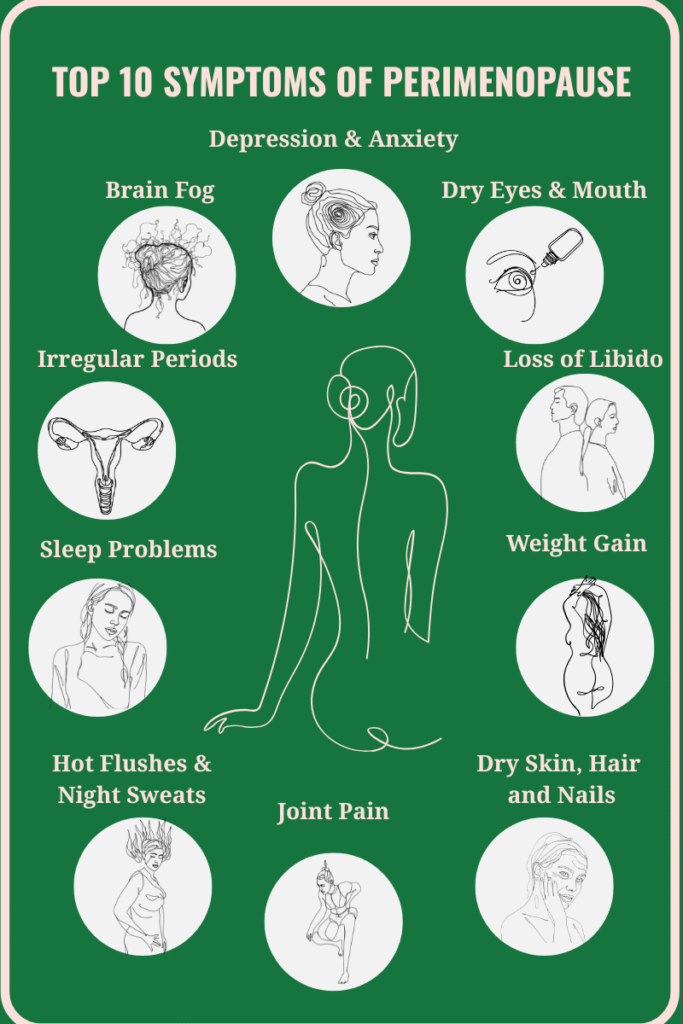
Are you in your 40s or 50s, eating well and exercising, but still battling frustrating belly fat, constant bloating, and fatigue?
You’re not alone, and it’s not your fault… it’s the hormonal shifts of perimenopause.
This transition, which can last for years before menopause, brings a cascade of changes that can make you feel like you’re fighting your own body.
This guide moves beyond generic diet advice. Written by a registered nutritionist with lived perimenopause experience, it provides a science-backed, gut-focused nutrition plan to manage your weight, beat bloating, and reclaim your energy.
I will translate the complex science of hormonal and metabolic shifts into simple, actionable steps.
The Science of Meno-Belly: Why Your Body and Gut Are Changing
To effectively manage the symptoms of perimenopause, it’s crucial to first understand the “why” behind them. The changes you’re experiencing aren’t a sign of failure; they are a direct physiological response to a new hormonal landscape.
By understanding these shifts, you can empower yourself with targeted strategies that work with your body, not against it.
The Oestrogen Effect: More Than Just Hormones
One of the defining features of perimenopause is fluctuating and ultimately declining levels of oestrogen. This hormone does much more than regulate your menstrual cycle. It plays a key role in how your body manages fat, uses energy, and responds to insulin. As oestrogen declines, your body’s entire metabolic system recalibrates.
Insulin Resistance & Weight Gain
This oestrogen decline is a primary driver of perimenopause weight gain. Your body may become less sensitive to insulin, a condition known as mild insulin resistance. This makes it harder for your cells to use glucose for energy, prompting your body to store more of it as fat, particularly around your abdomen. This stubborn central fat is often called the meno-belly.
According to Australian government health sources, these hormonal changes can lead to a shift in body composition, menopause involves significant hormonal changes — specifically falling oestrogen and progesterone — that lead to:
- increased body fat (especially abdominal),
- reduced lean muscle mass, and
- less efficient calorie burning.
Key Hormonal and Body Composition Changes

Hormonal Shifts: As oestrogen levels decline, the body experiences metabolic changes that make it easier to gain weight and harder to maintain muscle.
Body Composition: The loss of oestrogen causes fat to shift from the hips and thighs to the abdomen. This visceral fat is associated with increased risks of metabolic syndrome and type 2 diabetes.
Weight Gain: Women may experience an average weight gain of half a kilogram per year between ages 45–55.
Metabolic Rate: A lower metabolic rate means the body burns fewer calories, requiring adjustments to diet and physical activity levels
Your Gut on Perimenopause: The Microbiome Connection
If you’re suddenly dealing with constant bloating, gas, and digestive unpredictability, you’re not imagining it.
Perimenopause gut health is deeply intertwined with your hormones.
Oestrogen helps maintain the diversity and integrity of your gut lining and the trillions of microbes that live there. As hormones fluctuate, these microbiome shifts can lead to an imbalance, with less beneficial bacteria and more of the kinds that produce gas and inflammation. This is one of the most common bloating causes during this life stage. A less diverse microbiome can impair digestion, slow down gut motility, and compromise the gut barrier, contributing to systemic inflammation and worsening other perimenopause symptoms. Improving your digestive health is therefore not just about comfort; it’s a cornerstone of managing weight and overall well-being.
Core Nutrition Strategy 1: Master Your Macros for Metabolic Health
Fighting perimenopause symptoms requires a more strategic approach than simply eating less. Your body’s needs have changed, and your nutrition must adapt. By mastering your macronutrients protein, carbohydrates, and fats you can support your new metabolic reality, maintain muscle, and stabilise your energy levels.
Protein Pacing: Your #1 Tool Against Muscle Loss and Fat Gain
During perimenopause, protein becomes your most valuable player. The decline in oestrogen accelerates sarcopenia, the age-related loss of muscle mass. Since muscle is metabolically active (it burns more calories at rest than fat), this muscle loss can slow down your metabolic rate.
A higher protein intake helps counteract this in several ways:
- it provides the building blocks to preserve and build lean muscle,
- it requires more energy to digest (thermic effect of food), and it is incredibly effective for promoting satiety, helping you feel fuller for longer.
A key perimenopause nutrition strategy is “protein pacing, distributing your intake evenly throughout the day. Instead of a small amount at breakfast and a huge portion at dinner, aim for a consistent protein per meal target of 25-30 grams. This ensures your body has a steady supply of amino acids for muscle repair and helps prevent the blood sugar spikes and crashes that drive cravings. Download my High protein recipe eBook here

Smart Carbs and Strategic Fibre for a Happy Gut
Carbohydrates are not the enemy, but the type and timing matter more than ever. The goal is to choose smart carbohydrates, complex, high-fibre sources like whole grains, legumes, and starchy vegetables, over refined ones. These carbs release glucose into your bloodstream slowly, promoting stable blood sugar balance and preventing the insulin spikes that encourage fat storage.

Fibre is a superstar for both metabolic and digestive health. It’s crucial to understand the two main types:
Soluble vs insoluble fibre:
- Soluble fibre (found in oats, beans, apples, and carrots) dissolves in water to form a gel-like substance. It slows digestion, helps you feel full, and can lower cholesterol and blood sugar.
- Insoluble fibre (in nuts, whole wheat, and cauliflower) adds bulk to stool, promoting regular bowel movements and preventing constipation.
Proper fibre timing is also key. Introducing high-fibre foods gradually and ensuring adequate hydration can help your gut adapt without causing excess bloating.

Why a Mediterranean-Style Diet Work
Instead of a restrictive diet, adopting a Mediterranean diet pattern offers a sustainable and delicious framework for perimenopause. This approach is rich in fruits, vegetables, whole grains, legumes, nuts, seeds, and healthy fats like olive oil, with moderate amounts of fish and poultry.
The metabolic benefits of this eating style are well-documented. It naturally provides ample fibre, antioxidants, and anti-inflammatory compounds. Evidence, such as the landmark PREDIMED Mediterranean diet trial in NEJM supporting metabolic benefits, shows its powerful effect on improving insulin sensitivity and supporting long-term heart health, which becomes a greater concern for women post-menopause.

Core Nutrition Strategy 2: Targeted Gut-Health Interventions
With bloating and digestive distress being such prominent complaints, directly supporting your gut is a non-negotiable part of a successful perimenopause plan. These targeted strategies go beyond basic nutrition to calm an irritated digestive system and rebuild a resilient gut environment.
Prebiotics & Probiotics: A Food-First, Evidence-Led Approach
You can actively nurture your gut microbiome through diet. A food-first approach is the safest and most effective starting point.

Prebiotic foods are types of fibre that feed your beneficial gut bacteria. Excellent sources include garlic, onions, leeks, asparagus, bananas (especially slightly green ones), and oats. Including a variety of these foods helps the good microbes flourish.
Probiotics are live beneficial bacteria found in fermented foods like plain yogurt, kefir, sauerkraut, kimchi, and miso.
When it comes to perimenopause supplements, the probiotic market can be confusing. While some probiotic strains like Lactobacillus rhamnosus GG and Bifidobacterium lactis have evidence for supporting gut health, many products lack sufficient research. The NIH NCCIH evidence summary on probiotics and safety is a useful resource for understanding the science. Prioritise getting probiotics from food and consult a knowledgeable practitioner before spending money on supplements.
Step-by-Step Low-Bloating Meal Structure
How you eat can be just as important as what you eat. To create low bloating meals, focus on mindful assembly and timing. This approach eases the digestive load on your system, providing one of the most immediate bloating fixes.
- Anchor with Protein: Start with your 25-30g portion of lean protein (e.g., chicken breast, fish, tofu, Greek yogurt).
- Add Non-Starchy Vegetables: Fill half your plate with well-cooked, low-gas vegetables like zucchini, spinach, bell peppers, and carrots. Raw cruciferous vegetables (broccoli, cauliflower) can be gas-producing for some; steaming or roasting them makes them easier to digest.
- Include a Smart Carb Strategically: Add a small portion (about ½ cup cooked) of a smart carbohydrate like quinoa, sweet potato, or brown rice.
- Finish with Healthy Fat: Incorporate a serving of healthy fat, such as a tablespoon of olive oil, a quarter of an avocado, or a small handful of nuts or seeds.
- Practice Mindful Meal Timing: Avoid eating large, heavy meals late at night. Proper meal timing, such as allowing 3-4 hours between meals and not eating within 2-3 hours of bedtime, gives your digestive system adequate time to process food, reducing the likelihood of overnight bloating and discomfort.
The Gutsy Solution Menopause Plate

Your Action Plan: The 7-Day Clinician-Authored Perimenopause Meal Plan
Knowledge is powerful, but action creates change. To help you translate these strategies into your daily life, we’ve created the ultimate tool to get you started.
This downloadable 5-day meal plan is your roadmap to success. It takes all the guesswork out of what to eat, providing delicious, easy-to-prepare perimenopause recipes for breakfast, lunch, and dinner. Each day is designed to meet your protein targets, balance blood sugar, and incorporate gut-friendly foods. It also includes a complete shopping list to make your grocery store trip simple and efficient.
Here is a sample of what you can expect:
- Breakfast: Greek Yogurt Parfait with Berries & Chia Seeds (30g protein)
- Lunch: Chicken & veggie stir fry with brown rice (30g protein)
- Dinner: Grilled Salmon, Quinoa, Steamed Broccoli, Drizzle of Olive Oil (30g protein )
Authored by Gutsy Solution, a registered nutritionist with lived perimenopause experience, this plan is both scientifically sound and realistic for a busy life.
Beyond Diet: Supplements and When to See Your Doctor
While nutrition is foundational, a few supplements have good evidence for supporting women during perimenopause. Common perimenopause supplements to consider discussing with your doctor include:
- Magnesium: Can help with sleep, mood, and muscle relaxation.
- Vitamin D: Crucial for bone health, which is a concern as estrogen declines.
- Omega-3 Fatty Acids:** Have anti-inflammatory benefits that support heart and brain health. The
It’s vital to recognize when self-management isn’t enough. Certain menopause symptoms require medical attention. It’s time to know when to see a doctor if you experience any of the following:
- Severe mood swings, anxiety, or depression that interfere with your daily life.
- Persistent fatigue that isn’t improved by rest. *
- Heavy or irregular bleeding. *
- Heart palpitations. *
- Severe hot flashes or night sweats that disrupt your sleep and quality of life.
- Your doctor can discuss other options, including hormone therapy.
A Guide to Menopause provides lots of information and resources for perimenopause and menopause. You can alos get information from the Australian Menopause Society.
There are also a number of current practising medical doctors that provide free, up to date advice on menopause through their websites and social media including Dr Louise Newsome, Dr Naomi Potter & Dr Mary Clare Haver.
Managing perimenopause weight gain and bloating can feel like an uphill battle, but it is absolutely achievable with a targeted, gut-first nutrition strategy. Your body is not broken; it’s simply adapting to a new hormonal reality. By shifting your focus from calorie counting to nutrient quality prioritising protein, embracing strategic fibre, and nurturing your microbiome health you can empower yourself to take control of these changes. You can feel strong, energized, and comfortable in your body again. Your journey to a calmer gut and a healthier body starts now.
Download our exclusive 5-Day Perimenopause Rescue Meal Plan to begin today. For personalized support, consider booking a free 15-minute discovery call.
Frequently Asked Questions
This is a classic sign of perimenopause. The primary cause is declining estrogen, which changes how your body stores fat. It shifts fat distribution from the hips and thighs to the abdomen (visceral fat) and can also lead to mild insulin resistance, making it easier for your body to store calories as fat rather than use them for energy.
If you have to pick one, it’s protein. Prioritising protein is critical for fighting age-related muscle loss, which keeps your metabolism from slowing down. It’s also highly satiating, helping to control appetite and cravings, and it supports stable blood sugar levels.
Yes, absolutely. For many women, relief comes from *how* they eat, not just *what* they eat. Simple changes like managing fiber timing (e.g., cooking fibrous vegetables well), ensuring you’re well-hydrated, eating mindfully without rushing, and avoiding large meals late at night can significantly reduce bloating.
Not all, but many are marketed with claims that lack strong scientific evidence. The best approach is to start with food-first sources like plain kefir, yogurt, and sauerkraut. If you consider a supplement, look for products that specify the exact probiotic strains and have been studied in human clinical trials for the benefits you seek.
A general evidence-based guideline for active women in midlife is around 1.2 to 1.6 grams of protein per kilogram of body weight. However, a simpler and more practical target is to aim for 25-30 grams of high-quality protein with each of your three main meals. This “protein pacing” approach is highly effective for muscle maintenance and satiety.
Author Note This article was written by Gutsy Solution, a Registered Nutritionist (B. Nut Sc) who specialises in perimenopause and menopause nutrition. Her advice is informed by current clinical research and her own lived experience navigating the challenges of midlife hormonal changes. All scientific claims are anchored to high-authority research from institutions like the National Institutes of Health and leading medical journals but do not constitute medical advice.
Medical Disclaimer — Gutsy Solution
Important — Read Carefully
The information, content, materials, and resources provided by Gutsy Solution (including on our website, in emails, in printed materials, and in any digital or audio/video content) are for educational and informational purposes only and are not intended to be a substitute for professional medical advice, diagnosis, or treatment.
Not medical advice. Nothing provided by Gutsy Solution constitutes medical advice. Do not rely on our content to make decisions about your health. Always seek the guidance of a qualified healthcare professional with any questions you may have regarding a medical condition or treatment.