Why Menopause Changes Your Body
If you’re in your 40s or 50s and suddenly notice your waistline expanding despite eating and exercising the same way as before, you’re not alone. Many women describe thier menopausal weight gain as if a balloon inflated in their midsection overnight. Clothes no longer fit the same, energy levels dip, and frustration grows.
Here’s the important truth: nothing is wrong with you. These changes aren’t a sign of weakness or failure – they’re the predictable result of hormonal changes during perimenopause and menopause. It has nothing to do with your willpower or letting yourself go or being lazy.
Weight gain in midlife isn’t just about the number on the scale. It’s about shifts in body composition, metabolism, and fat distribution. Understanding these changes is key to managing them — and the good news is, there are proven strategies to help.
What Exactly Is “Menopause Belly”?

When people talk about “meno-belly” or “menopot,” they’re describing a specific pattern of fat gain that occurs during the menopausal transition.
Unlike general weight gain, this belly fat often develops even when a woman’s overall weight doesn’t change. In fact, many women report that while their arms and legs get thinner, their waistline grows larger. They also often say that they are not doing anythig different, their diet and excerise hasnt changed at all but their weight keeps increasing and they can’t lose the weight the way they used to in their 20’s or 30’s.
Subcutaneous vs. Visceral Fat
Subcutaneous fat sits directly under the skin. It’s soft and pinchable — the “muffin top” that spills over waistbands. While annoying, it’s less concerning for long-term health.
Visceral fat, the weight gain we often see on our bellies in menopause, on the other hand, is far more dangerous. It lies deep inside the abdomen, wrapping around vital organs like the liver, intestines, and stomach. Unlike subcutaneous fat, visceral fat is metabolically active, releasing inflammatory substances that disrupt health.
Why Visceral Fat Is More Dangerous
Visceral fat isn’t just a cosmetic issue — it’s a metabolic one. It increases the risk of:
- Cardiovascular disease
- Type 2 diabetes
- High blood pressure
- Insulin resistance
- Certain cancers
That’s why many healthcare providers measure waist circumference or waist to hi ratio as an indicator of disease risk. A growing belly during menopause isn’t just about how you look — it’s about what’s happening inside your body.
The Science Behind Menopausal Weight Gain

Menopausal weight gain is driven by a complex interplay of hormones, metabolism, and ageing. Let’s break it down.
Hormonal Changes Driving Fat Redistribution
Oestrogen Decline
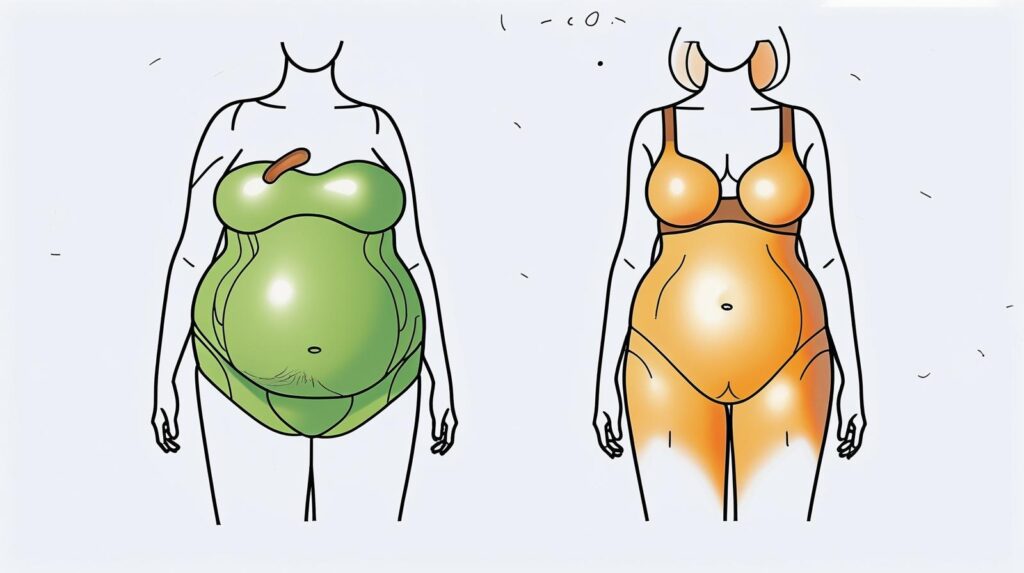
Oestrogen regulates metabolism and fat storage. In reproductive years, it directs fat toward the hips and thighs (the “pear shape”).
But as estrogen declines, fat storage shifts to the abdomen, resulting in an “apple shape.”
Increased Availability of Testosterone
With lower oestrogen, testosterone becomes more dominant. This hormonal imbalance encourages abdominal fat accumulation, making belly fat almost inevitable for many women.
Changes in Hunger Hormones
Leptin is a hormone your body releases that helps it maintain your normal weight on a long-term basis. The level of leptin in your blood is directly related to how much body fat you have. Leptin resistance causes you to feel hungry and eat more even though your body has enough fat stores.
Ghrelin is a hormone your stomach produces and releases. It signals your brain when your stomach is empty and it’s time to eat. Ghrelin levels increase between mealtimes and decrease when your stomach is full. People who have obesity often have low ghrelin levels, while people who significantly restrict their calorie intake have high ghrelin levels.
Leptin levels decrease, reducing natural appetite suppression.
Ghrelin levels rise, especially with poor sleep, increasing hunger and cravings.
This hormonal shift explains why many women feel hungrier and have a harder time controlling food intake during menopause.
Metabolic Slowdown
Research1 shows that women who transition to menopause experience:
- A 32% reduction in fat burning (oxidation)
- A 1.5x greater decline in energy expenditure during sleep
This means your metabolism is slower, even when you’re resting.
Muscle Mass Decline and Its Role in Weight Gain
Muscle burns more calories at rest than fat. Unfortunately, menopause accelerates muscle loss:
- After 50, women lose 5–10% of muscle mass every decade.2
- The SWAN study found that lean muscle declines while fat accumulation doubles during menopause.3
Less muscle means fewer calories burned, which makes weight gain easier and weight loss harder.
Inflammation and Fat Tissue Dysfunction
Menopause isn’t just about fat gain — wjhit’s about changes in the fat tissue itself. Research shows that postmenopausal women experience:
- Larger fat cells (adipocyte hypertrophy)
- Increased inflammation
- Fibrosis (scar tissue in fat cells)
This makes fat tissue metabolically unhealthy, driving insulin resistance and worsening belly fat.4
Numbers That Tell the Story

- 65.5% of women aged 40–59 have abdominal obesity
- 73.8% of women aged 60+ have abdominal obesity
- Average weight gain during menopause transition: 10kg (22 lbs)
- Visceral fat doubles from 5–8% to 10–15% of body weight
These numbers highlight why menopausal weight gain isn’t an isolated experience — it’s nearly universal.
Health Risks of Menopausal Weight Gain
Belly fat during menopause isn’t just frustrating — it’s dangerous.
Heart Disease and High Blood Pressure
Visceral fat releases inflammatory cytokines that damage blood vessels and raise blood pressure. This significantly increases the risk of heart disease, the leading cause of death in women.
Type 2 Diabetes and Insulin Resistance
Belly fat promotes insulin resistance, making it harder for the body to regulate blood sugar, increasing the risk of type 2 diabetes.
Cancer, Dementia, and Metabolic Syndrome
Research links abdominal obesity to higher risks of breast cancer, colorectal cancer, and even dementia. It also contributes to metabolic syndrome — a cluster of conditions including high blood pressure, high blood sugar, and abnormal cholesterol.4-7
Whilst understanding the science behind menopausal weigh gain and its associated health risks is the first step, the good news is ther aree proven, practical strategies to help prevent or reduce it.
In our next post, we’ll dive into the evidence-based solutions – covering nutrition, exercise, hormone therapy, and lifestyle interventions – that can make a real difference during the menopause transition.
Stay tuned for Part 2, where we’ll focus on what actually works to support your health, energy and confidence.
References
- 1. Lovejoy, J. C., Champagne, C. M., de Jonge, L., Xie, H., & Smith, S. R. (2008). Increased visceral fat and decreased energy expenditure during the menopausal transition. International journal of obesity (2005), 32(6), 949–958. https://doi.org/10.1038/ijo.2008.25
- 2. Mitchell, W. K., Williams, J., Atherton, P., Larvin, M., Lund, J., & Narici, M. (2012). Sarcopenia, dynapenia, and the impact of advancing age on human skeletal muscle size and strength; a quantitative review. Frontiers in physiology, 3, 260. https://doi.org/10.3389/fphys.2012.00260
- 3. Harlow, S. D., Burnett-Bowie, S. M., Greendale, G. A., Avis, N. E., Reeves, A. N., Richards, T. R., & Lewis, T. T. (2022). Disparities in Reproductive Aging and Midlife Health between Black and White women: The Study of Women’s Health Across the Nation (SWAN). Women’s midlife health, 8(1), 3. https://doi.org/10.1186/s40695-022-00073-y
- 4. Abildgaard, J., Ploug, T., Al-Saoudi, E., Wagner, T., Thomsen, C., Ewertsen, C., Bzorek, M., Pedersen, B. K., Pedersen, A. T., & Lindegaard, B. (2021). Changes in abdominal subcutaneous adipose tissue phenotype following menopause is associated with increased visceral fat mass. Scientific reports, 11(1), 14750. https://doi.org/10.1038/s41598-021-94189-2
- 5. UK Biobank 2023
- 6. Lizcano, F., & Guzmán, G. (2014). Estrogen Deficiency and the Origin of Obesity during Menopause. BioMed research international, 2014, 757461. https://doi.org/10.1155/2014/757461
- 7. Davis, S. R., Castelo-Branco, C., Chedraui, P., Lumsden, M. A., Nappi, R. E., Shah, D., Villaseca, P., & Writing Group of the International Menopause Society for World Menopause Day 2012 (2012). Understanding weight gain at menopause. Climacteric : the journal of the International Menopause Society, 15(5), 419–429. https://doi.org/10.3109/13697137.2012.707385